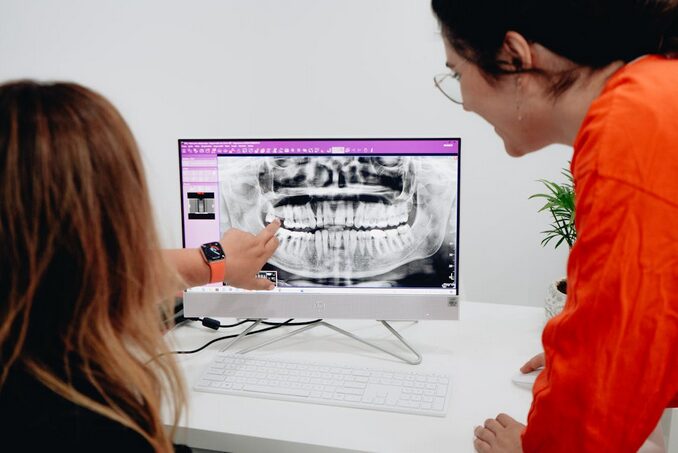
Dental pain and untreated infections can quickly escalate into serious oral health issues if not addressed in time. Endodontic care focuses on diagnosing and treating problems within the tooth’s inner structures, helping to save natural teeth and prevent further complications. Seeking care from a professional endodontist glendale ca ensures that infections are properly managed through procedures like root canal therapy. This targeted treatment removes bacteria, relieves pain, and protects surrounding teeth and tissues from damage. By addressing issues early, endodontic care plays a vital role in maintaining long-term oral health. This article explores how these treatments help prevent more severe dental complications.
Preventing the Spread of Infection

Preventing the spread of infection beyond the affected tooth is one of the most crucial aspects of endodontic treatment. Abscesses, or pockets of pus that grow at the tooth’s root, can result from an infected pulp if treatment is not received. These infections may spread to the surrounding soft tissues and bone, leading to severe discomfort and swelling. The infection may also spread to other parts of the body in extreme circumstances. By removing contaminated tissue and cleaning the root canal system, endodontic therapy effectively controls the condition and prevents it from progressing to a more serious health issue.
Preserving Natural Teeth and Oral Structure
 Endodontic care is essential for preserving natural teeth that might otherwise require extraction. Maintaining the natural tooth structure helps support proper chewing function, alignment, and overall oral stability. When a tooth is removed, it can lead to the shifting of neighboring teeth and changes in bite alignment, which may create additional dental issues over time. By saving the tooth through procedures such as root canal treatment, endodontic care helps maintain the integrity of the dental arch. This preservation reduces the need for more complex restorative solutions and supports long-term oral health.
Endodontic care is essential for preserving natural teeth that might otherwise require extraction. Maintaining the natural tooth structure helps support proper chewing function, alignment, and overall oral stability. When a tooth is removed, it can lead to the shifting of neighboring teeth and changes in bite alignment, which may create additional dental issues over time. By saving the tooth through procedures such as root canal treatment, endodontic care helps maintain the integrity of the dental arch. This preservation reduces the need for more complex restorative solutions and supports long-term oral health.
Reducing Pain and Preventing Chronic Conditions
Infections within the tooth pulp can cause significant discomfort, including persistent toothaches, sensitivity, and swelling. Endodontic treatment addresses the underlying cause of this pain rather than simply managing symptoms. By removing inflamed or infected tissue, the procedure alleviates discomfort and prevents the development of chronic dental conditions. Untreated infections can lead to ongoing inflammation and recurrent pain, affecting quality of life. Timely endodontic care ensures that these issues are resolved effectively, reducing the likelihood of recurring problems and long-term complications.
Supporting Overall Oral and Systemic Health
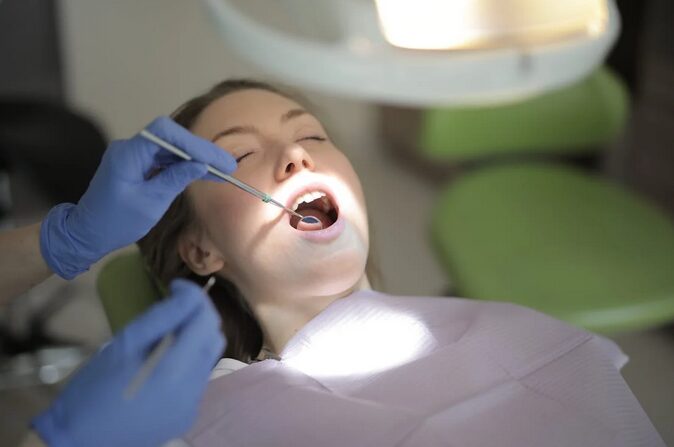
Oral health is closely connected to overall health, and untreated dental infections can have broader implications. Bacteria from oral infections may enter the bloodstream and contribute to systemic health concerns. Endodontic care helps eliminate these sources of infection, supporting not only oral health but also general well-being. By maintaining a healthy oral environment, patients reduce the risk of complications that could affect other parts of the body. This connection underscores the importance of promptly and effectively addressing dental issues through specialized care.
Endodontic care plays a vital role in preventing serious dental complications by addressing infections at their source, preserving natural teeth, and supporting overall health. Through procedures that remove infected tissue and restore function, this form of treatment helps avoid the spread of infection, chronic pain, and structural damage. By maintaining the integrity of the tooth and surrounding tissues, endodontic care contributes to long-term oral stability and well-being. Its importance extends beyond immediate relief, making it a key component of comprehensive dental care.